2024 – Norah Jade Robinson-Kerr
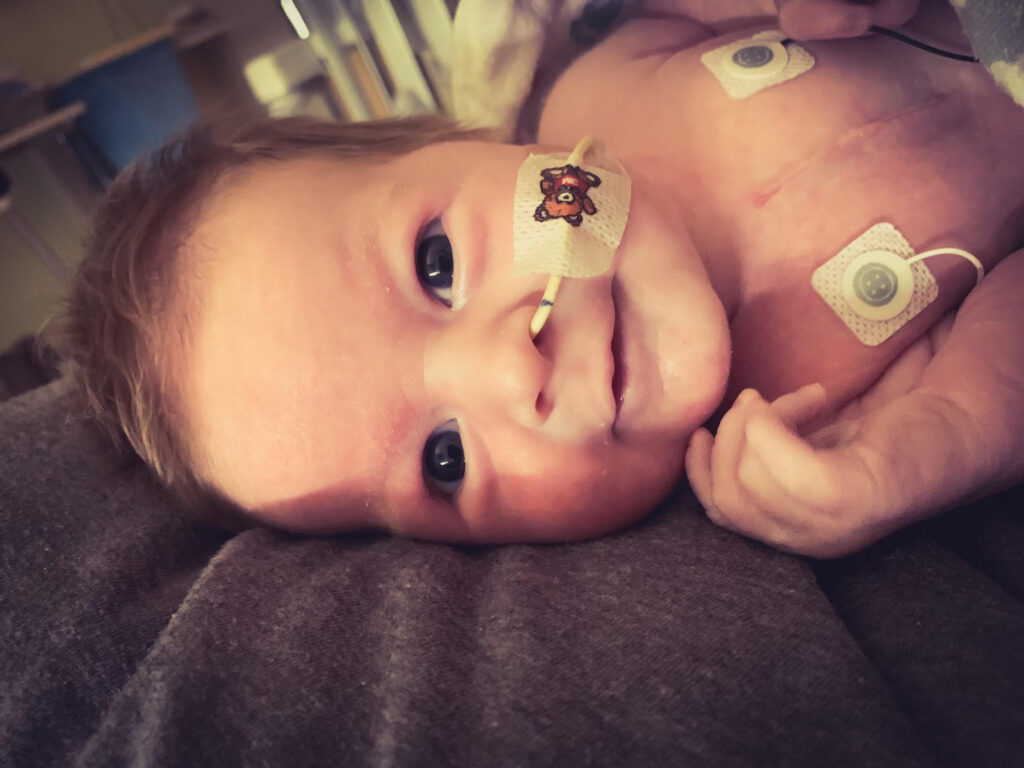
Lauren Robinson is a single mother raising her daughter, Norah, with the help of her incredible boyfriend, Travis Kerr. Lauren gave birth to Norah in March, 2020. It was a very difficult pregnancy. Lauren felt something was wrong throughout the pregnancy. She had numerous visits to the doctor, expressing great concern and explaining how she could not feel the baby. Each time she was discharged with the assurance that the baby is fine and in good health. At 36 weeks, she arrived at the hospital’s ER complaining of excruciating back pain. Lauren kept insisting that something was wrong. The medical staff and the doctors determined that there was, in fact, a problem. Norah’s heart rate was very low and she was in significant distress. After several hours, an emergency cesarean section was performed. On March 11, 2020, Norah was born at 4 pounds 3 ounces. The medical professionals discovered that Lauren had blood clots in her placenta. They also discovered suspicious areas of Norah’s brain. The doctors then decided to transfer them to Children’s Hospital in Denver, Colorado. Upon their arrival at Children’s Hospital, Norah was given an MRI. The neurology team delivered the wrenching news that Norah had experienced a stroke in the womb and her brain had been oxygen-deprived for an extended period of time, resulting in significant brain damage.
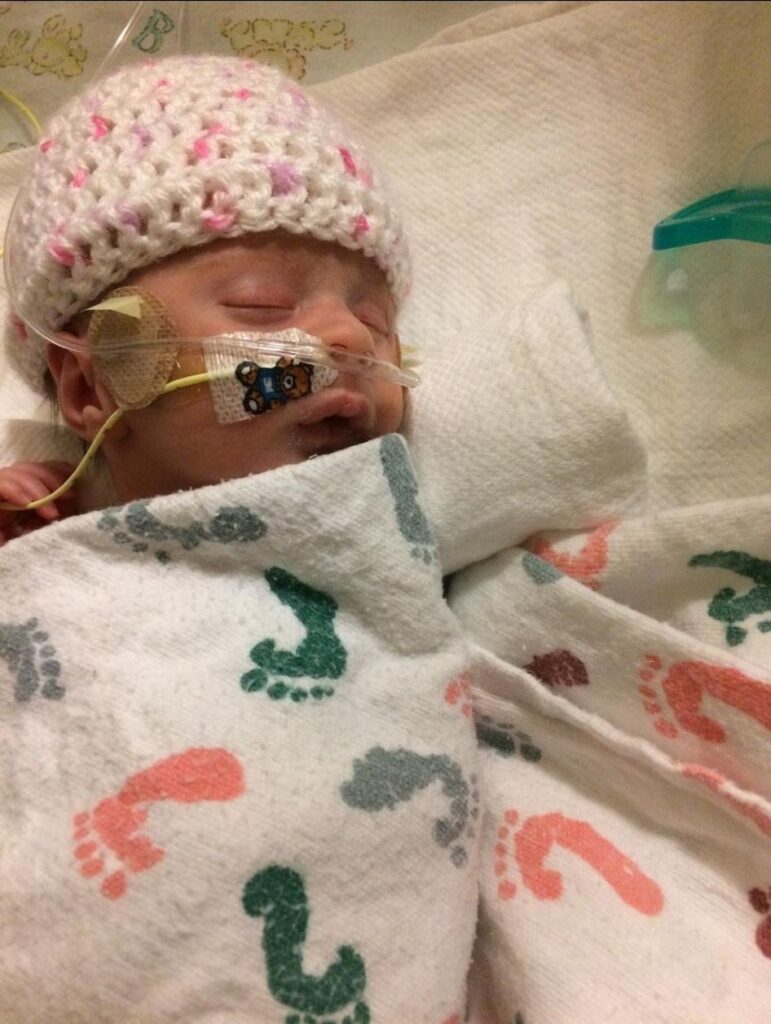
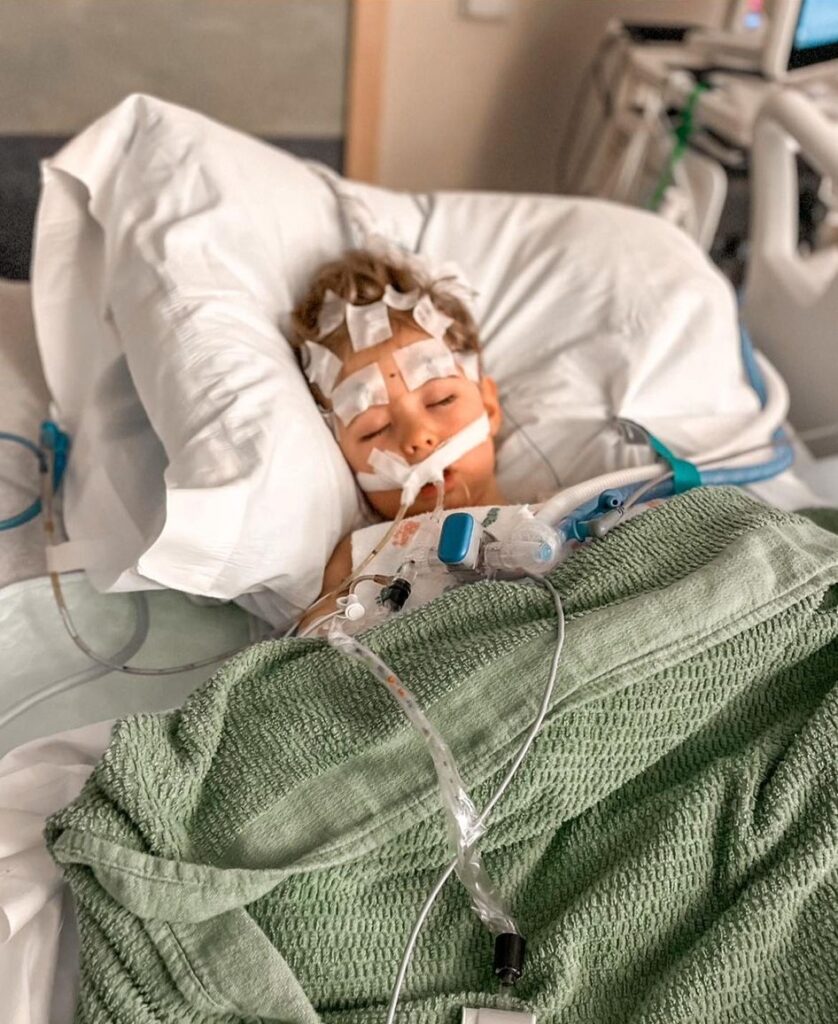

Her condition was identified as Hypoxic Ischemic Encephalopathy. The doctors explained to Lauren that they did not know what Norah’s future would look like. Despite all of Norah’s issues the first three years, she excelled in her therapies and was able to reach some huge milestones in her own time. Norah began to do things that were said she would never do. Tragically, in February, 2023, Lauren and Norah were were struck from behind by another vehicle in what appeared to be a minor accident. Unfortunately shortly after being rear-ended, Norah experienced a very severe and prolonged seizure. Norah had never had a seizure before and at the sight of this horrifically, horrible seizure Lauren moved fast to call 911 and pull over to get help. An ambulance arrived and took Norah to the emergency room. When Lauren got there, one of the staff members was using a bag to breathe for Norah. The medical professionals were getting ready to insert a breathing tube so that Norah could be put on a ventilator to save her life. After that, Norah was taken by helicopter to the intensive care unit of Children’s Hospital so that she could receive life-saving procedures. In 48 hours, little warrior Norah started breathing on her own. A week later, she was discharged. Sadly, this was a major set-back to Norah’s development, and she has not gone back yet to where she was developmentally. She now has another diagnosis of a severe and rare form of Medication Resistant Epilepsy, causing Norah to have three to five seizures per hour. This added to her many other medical conditions of Cerebral Palsy, and severe muscle spasms. Her extremely painful muscle spasms are very difficult to control with a helpless feeling of bringing comfort to Norah. Along with all the medical conditions that Norah lives with, she is also legally blind (can see some colors) and must eat and drink through a feeding tube. Both Lauren and Travis work hard to make Norah comfortable, cared for and happy. They desire for Norah to feel the most loved possible, despite being medically fragile. Travis suffered a spinal cord injury in 2005, leaving him wheelchair bound for the rest of his life. He has such a tender, compassionate and loving heart for Norah. Lauren is Norah’s full time CNA caregiver. She provides for Norah’s around-the-clock care and attention.


Norah just celebrated her fourth birthday. Over the past four years Lauren, and now Travis, are dedicated to giving Norah the best care and most love possible. They are doing everything possible to help Norah regain her progress that was lost after the first seizure. Every day with Norah is a blessing! Although she is plagued with a myriad of physical symptoms and disabilities, you can look into her eyes and see the warrior within her. She is a portal of love and her gentle soul melts the hearts of all that meet her.
2023 – Slade Eastberg & Owen Cannady
We’re so excited to have TWO families in 2023! Here are there stories:
OWEN CANNADY

Chelsea and her husband, Richard, have four children. 9 year old twins Brooke and Carson, 2-year-old Wyatt, and their newest addition Owen who is 3 months old.
24 weeks into Chelsea’s pregnancy with Owen her ultrasound identified a heart defect in her baby boy. The heart defect, Dextro-Transposition of the Great Arteries (d-TGA). d-TGA is a birth defect where the two main arteries of the heart, the pulmonary and aorta artery, are switched in position. This is a fatal heart defect if not immediately addressed at birth.
Chelsea went into labor mid-November, and the doctors were able to stall the labor, but she did have to live at the Ronald McDonald house close to Children’s Hospital because labor could come at any time. The were thankfully able to stall his birth until her due date and she was induced December 4th and Owen was born on December 5th. Labor went about as well as to be expected and Owen was taken immediately for his first procedure, followed by another on day 5 which was the open heart surgery to address the swapped ventricles in his heart. Owen handled the surgeries like a champ and after 3 weeks in the hospital, he got to go home celebrate Christmas at home with his family. Since then, he’s had several follow up appointments and is doing well.
They have since been able to take him off oxygen with close monitoring of course and he has overcome a potential concern of fluid around his heart. He does have Supra Ventricular Tachycardia or SVG which is being medicated and monitored closely. He will continue to need frequent visits to Children’s Hospital for cardiologist appointments and checkups.
During this challenging pregnancy, Chelsea did lose her job of 6 years which their family of 6 was dependent on to supplement Richard’s income to make ends meet. Richard had to use many weeks of unpaid FMLA to be there for Chelsea and the baby pre and postpartum, as well as to care for their other 3 children back at home. Chelsea still hasn’t been able to return to work and it’s unknown when or if that will be possible.
Owen Richard is the true definition of a miracle. He is going to do amazing things!!! He is so loved!!!
SLADE EASTBERG
Jordyn and Bret Eastberg have 3 sons -10 year old Brayden, 5 year old Tucker, and 2 year old Slade. Jordyn had a fairly straightforward pregnancy, aside from a little extra amniotic fluid that would be monitored throughout. At 38 weeks, they decided to induce due to a major increase of those fluid levels and risks involved with waiting for labor to come naturally. After induction, her labor and delivery went perfectly and baby Slade appeared to be a happy, healthy baby, but they quickly learned that wasn’t the case. Slade was gasping for air and turning blue from lack of oxygen. He was rushed to the NICU where after several tests they discovered that Slade’s esophagus wasn’t connected to his stomach and his trachea and esophagus had an abnormal connection; called Esophageal Atresia (EA) and Tracheoesophageal Fistula (TEF) respectively. He could not survive without almost immediate surgery. So, only hours after giving birth, Jordyn and Bret followed an emergency ambulatory transport for Slade to Children’s Hospital. The next morning, Slade had his first surgery to repair these issues.
The next day, doctors noticed the problems didn’t end there. Slade was in active heart failure due to a Congenital Heart Defect (CHD) where he had a large hole in the lower two chambers and several smaller holes as well as a coarctation, his main artery was closing. For the next several weeks at Children’s, Slade was on a heart medication, IV for nutrition, and a ventilator until they could perform an open heart surgery. After the surgery, one of his chest tubes fell out and he began to plummet and his lung collapsed for which they performed yet another emergency. Doctors knew at this point after so many issues they needed to thoroughly check Slade from head to toe for more concerning problems. They found vertebrae abnormalities called Butterfly Vertebrae, fused ribs and extra ribs. Because of all these combined issues, doctors diagnosed Slade with VACTERL, explained simply as a very rare set of physical abnormalities that occur together. When a child has 3 or more of these anomalies (V(Vertebrae)A(Anal Atresia)C(cardiac defects)TE(TEF/EA)R(renal defects)L(Limb Differences)) that cannot be linked to other genetic issues, the child receives this diagnoses. The hardest part about the diagnoses is that you never know when the next “thing” will come. They know already that Slade has the V, C, and TE. During his initial esophagus surgery, his vocal cords were paralyzed requiring a G tube, this was supposed to be temporary but he still has to use it to this day. Around 6 months he still couldn’t pass a swallow study and was diagnosed with Laryngeal Cleft that would also need surgery to repair. The first repair surgery for the cleft didn’t hold and he had to have it a second time. He also has been diagnosed with Tracheomalacia weakening his airway which is particularly problematic when he is sick. He just had his second open heart surgery in January, and another esophagus surgery in December. He will continue to need additional esophagus dilations for the rest of his life. After two years of severe reflux and daily vomiting, he was diagnosed with a hiatial hernia which will require yet another surgery soon. They don’t know what will come from his Vertebrae issues or if he will ever be able to get off his G-tube. The unknowns of Slade’s future are overwhelming for Jordyn and Bret.
Slade spent his first 8 weeks at Children’s and got to go home and meet the rest of his family and brothers for the first time! Jordyn was only given 8 weeks of leave from her job so the weekend after bringing Slade home, she had to prepare to return to work. Bret is self-employed and was trying to balance caring for Slade and doing his job while Jordyn was at work and they quickly realized it just wasn’t sustainable and she had to make the decision to leave her career. Thankfully, she was able to obtain her CNA license about 6 months ago so she can take care of Slade full time as he needs and earn some income to help make ends meet. Slade has recently started walking thanks to his ankle braces, he has started speaking and laughing which is a joy they weren’t sure they’d ever get to hear after his vocal cord paralysis. They are currently waiting on referral to Children’s Hospital in Boston, because there is not a doctor at Aurora Children’s Hospital for the TEF/EA issues that Slade has. They will have to travel to Boston once approved which presents a whole new set of financial worries. He’s had and will continue to have countless procedures, evaluations, medications, hospitalizations, and therapies likely for the rest of his life.
Slade’s story is one of perseverance, miracles, and lots of love.
2022 – Gavin Bond
Gavin was diagnosed when before birth with Tetralogy of Fallot, a critical congenital heart defect (CHD) consisting of 4 defects. He would require open heart surgery to survive. He was also diagnosed with hydronephrosis, a condition in which there is water on the kidneys.
This sweet boy was born at 37 weeks in November of 2016. He was 7 lbs 8oz and 18” of absolute cuteness. But he was sick, and was immediately put on a CPAP and heart monitor. He couldn’t coordinate his suck/breathe/swallow reflex, so he was quickly given an NG tube. He eventually gained the ability to eat, but continued to require 24/7 oxygen, but after only 8 days he was able to go home with his family.
A few weeks later, he was having trouble keeping his oxygen up. After a call to cardiology, he was brought back to the emergency room at Children’s Hospital. His heart was sick, and it was determined that he would need surgery. He was just 5 weeks old at the time of his first open heart surgery.
The surgery was rough, but he made it through, but recovery was much worse. He was intubated for 4 days because one of his lungs had collapsed. A week later, they found out that he had a stroke during surgery. Because of the stroke, he couldn’t eat without aspirating, so before he was discharged 3.5 weeks after his open heart surgery, he had one more surgery to have a g-tube placed.
Once he recovered a bit more, we were still concerned. He still seemed unwell. His lips and feet and the tip of his nose would turn blue. He slept like a newborn, but he was 5 months old and he was severely underweight. At his cardiology appointment that month, we were told he would need another open heart surgery, and our hearts broke. The doctors first tried to do a catheterization to see if they could avoid the surgery, but it wasn’t successful, so when he was 6 months old, he underwent another open heart surgery. There were some further bleeding complications, but he didn’t have another stroke, so that was wonderful! He came home after only a week this time around.
Since then, its been up and down with Gavin’s health. They had about 2 years where the biggest battle was Gavin’s growth. They could not get him to gain weight and eventually his g-tube was converted to a gj-tube and he did gain a little weight, but not enough.
Then, in January of 2021, Gavin had an MRI. At that time, it was determined he had a tethered spinal cord and a Chiari malformation. He had back surgery the following month to detether his spinal cord. That was a difficult recovery as he lost the ability to walk for a week and a half, but like he always does, he recovered.
In May of 2021, he was scheduled to have some more surgery. Because he has severe sleep apnea, they were going to take out his adenoids and do a nasal turbinate reduction. But, a few days before surgery, he tested positive for COVID, so surgery was delayed until June. That was a difficult recovery as well and Gavin’s anxiety has gone through the roof where hospitals and doctors are concerned.
He, again, recovered like a champ. But in February of 2022, he needed some more surgery to remove a lingual tonsil and to redo the nasal turbinate reduction. He was also tested for growth hormone deficiency because despite having incredible weight gain over the past year, his height has not changed and his medical team is becoming concerned. Turns out he is growth hormone deficient and will begin growth hormone therapy in the coming weeks. He may need brain surgery to address his Chiari malformation, and they may fix his deviated nasal septum. He is also expected to have his 3rd open heart surgery in the next year or two.

You’d never know by looking at him that this is his life experience. He is outgoing, smart, funny, sweet, and so handsome. He is a wonderful child who continues to grow and learn, all while facing a scary and uncertain future. And he does it with grace and maturity far beyond his 5 years. Gavin is a warrior!
2020 & 2021 – Wild Family Story
UPDATE: Our board has decided to roll our 2020 beneficiary family into 2021, since most of our events for 2020 were canceled due to COVID-19.

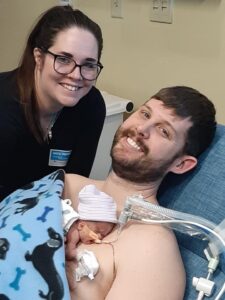
Cody and his five-year-old daughter Reese, along with Beca and her eight-year-old daughter Mackenzy, became a blended family in 2019, following a whirlwind romance that began in June of 2018. After much personal deliberation, Cody and Beca, with the approval of Mackenzy and Reese, decided to expand the family by having a child together. All four members of the fledgling family were thrilled with the prospect of bringing a new little one into the fold.
On witnessing the initial ultrasound, they discovered that they were going to be welcoming two new members to the family, and not just one! After the initial shock of the discovery, they realized that they would not have enough room in their current home, so they started searching for a home that would accommodate a six-person household.
After a few more ultrasounds, the doctor notified the Wilds that the babies might be suffering from twin-to-twin transfusion syndrome, a condition where there is a flow imbalance between the twins, causing the donor twin to have decreased blood volume, diminished development and growth, and also decreased urinary output, the result of the last item being a reduced or lower-than-normal amount of amniotic fluid. They were eventually referred to a specialist in Denver.
In December, at eighteen weeks pregnant, the Wilds became first time homeowners.
On December 18th, 2019, they made the trek to Denver to meet the new (referred) physician. They were both fearful and hopeful. The doctor confirmed that the twins were, in fact, suffering from twin-to-twin transfusion syndrome, and they were in stage two of five. It was relatively early, but they would have to act quickly. The boys very survival depended on it. Immediate surgery was imperative. The surgery was scheduled for the week of December 23rd, and a highly regarded fetal surgeon was flying in from Seattle to perform the necessary surgery. As fate would have it, staffing in the Denver facility was not sufficient to schedule the surgery during that week, and the Wilds were informed they would have to travel to Seattle. They piled into the car on December 21st, and headed for Seattle for the procedure, a fetal laser ablation, scheduled for December 23rd. The surgery went smoothly, and Beca was released the following day. They decided it was time to name the boys. Ryder Eugene (recipient baby) and Brody James (donor baby). After the surgery, there were many more frightening moments. It seems that during the laser ablation surgery, Ryder’s amniotic sac was compromised with a hole, complicating matters yet again. The twins needed to hang on and stay in the womb until twenty-four weeks, in order to be admitted to the Neonatal Intensive Care Unit (NICU) and to continue developing as much as possible in the womb. Beca was put on bedrest, and therefore was not able to work. The out-of-pocket expenses were mounting, and they were down to one elementary school teacher’s income.
On February 6th, following this crazy roller-coaster ride, the pregnancy was finally considered viable, and Beca was admitted to the hospital on February 8th. Within minutes of being admitted, Ryder’s heartbeat dropped to 70 bpm. The likelihood that both boys would survive was so small that Cody and Beca had to make the wrenching, nearly instantaneous decision to allow Ryder to pass, so that his brother Brody might have life. Ryder passed peacefully at 5:00 p.m. on February 8, 2020.
On February 16th, Brody arrived, at a whopping 1.8 pounds and 12” long! 

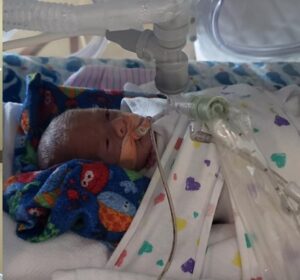
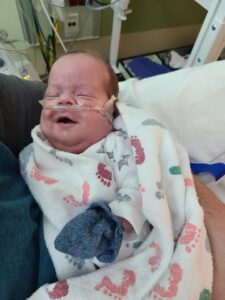
Brody was diagnosed with a Patent Ductus Arteriosus (PDA) a tiny hole in the heart, and on March 5th, he underwent surgery to repair the PDA. Unfortunately, during the surgery, Brody’s tricuspid valve was damaged. The damage healed itself, but the nature of this issue is that it will be necessary for him to see a cardiologist regularly for the duration of his life. He also has a brain bleed that is being closely monitored. Brody is improving steadily, gaining weight, improving function, breathing well and greatly impressing his caregivers in the NICU! He isn’t home yet, but is steadily progressing in that direction. Cody, Beca, Mackenzy and Reese cannot wait to welcome him home and start life in their new home with Brody Eugene Wild as a most important piece of the family puzzle!

2019 – Olivia & Barrett Family Story

Casey and Kiely Barrett met in 2003 in Arizona. They had their first child, Jordan in 2005. He has been diagnosed with high functioning Autism. Despite his social difficulties, he is a pretty happy kid now in middle school. He is a LEGO expert, and he loves his sister.
Kiely and Casey also had a second son in 2007, CJ. CJ was born with numerous neurological abnormalities. He functioned at about a 2 month infant level of development for most of his life. Sadly, he passed in 2010 at the age of 3.
After CJ’s passing the family got a dog. A Siberian Husky named Jethro, who has become emotional support for the whole family, being that he is a big fluffy goofball.
Shortly after that, they had a daughter in 2011, who they named Olivia (all of the children have been named after family members). Because of CJ’s developmental and neurological issues, Olivia was monitored and tested for many things at birth. Unfortunately, she was born with many similar abnormalities as CJ. She is on multiple seizure medications, and requires constant care. The prognosis for most kiddos like CJ and Olivia is a life span of about two years.
This June, Olivia will turn eight years old. She also functions at about a 1-2 month old infant. However, she is almost 50 lbs and non-ambulatory, it has become increasingly more difficult for the family to be able to transfer her to different places. Since she only continues to grow, at some point will be even more difficult for everyone to be able to transfer her in and out of her wheelchair to things like her bed, her bath chair, and her car seat. She is also scheduled for a dual hip surgery and will be hospitalized for a week during the summer of ’19.
In 2015, at the age of 37 years old, Kiely had a series of small strokes (not ATIs, but strokes) and was hospitalized. She has since made a decent recovery, but will be on some form of medication and will be monitored for the duration of her life.
Casey is Olivia’s parent CNA through her Medicaid waiver. He is mostly the stay at home dad, but also has a second full-time job working overnights. He also volunteers at Children’s Hospital and numerous other charitable events as Batman, and has done so for the past three years.
The Barretts have been blessed with a loving family support system, who has been there for numerous set backs that life has thrown their way. Since CJ’s passing, there have been many of those set backs to the point that the family has had to move seven times in the past nine years. Twice where they were technically homeless and had to move in with family, while commuting their children to school, sometimes to the tune of eighty miles per day. They have been fortunate to have family to help them through this life and the cards that have been dealt to them. Everything from stolen vehicles, loss of jobs and homes, to support when CJ and Olivia have spent significant time in the hospital.
2018 – Penelope’s Story
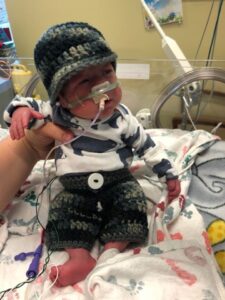
Penelope Sue Birgen is Leah and Jeff’s third baby. They also have two sons, ages 5 and 3. Penelope was born with three heart defects, significant lung damage, no spleen, and would eventually need GI surgery due to feeding and digestion difficulties. Penelope turned 1 on February 14, 2018 and she has already undergone 4 open heart surgeries, numerous cardiac catheterization procedures, extensive GI surgery, has been on ECMO three times, intubated for over a month, required blood transfusions, and countless x-rays, MRIs and CT scans. Most recently she has been recovering from meningitis which resulted in her flat lining and needing 35 minutes of CPR to revive her. While her family lives in Loveland, Colorado Penelope spent 156 days at Boston Children’s Hospital. Only recently (February 15, 2018) being transferred back to Colorado Children’s hospital via a private Medical Flight Team.

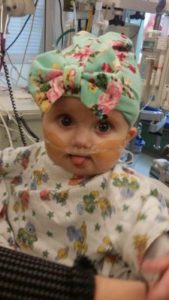
Penelope reaching the milestone of 1 year old was something many medical professionals believed she would not reach. She has spent over half her life in hospitals away from home so Jeff and Leah have needed to rely on help from family and friends to watch over their other two children so Leah could stay at Penelope’s bedside and Jeff could work. Leah had to leave her job and the family has needed to borrow money and take on credit card debt in order to continue to provide for the family and pay medical and prescription bills.

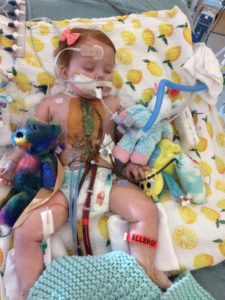
This family has been on a rollercoaster ride for the last year. The day to day stressors of work, childcare, bills and more bills compounded with the fight for Penelope merely surviving the day has been unimaginable. Somedays it feels as if all will be okay and other days they are grasping to hope. Two things are true: first, Penelope is an amazing little girl with a purpose! She lived when they said she wouldn’t! She does things on her own time but she continues to thrive even when odds are stacked against her. This little girl has changed the lives of so many around her! Second, living this life would take its toll on anybody and while the Birgens have low days, they live this life with such beauty and grace! This family celebrates every day as a gift. They look at the road ahead and without question, forge forward! This little girl is a fighter and so is her family.
2017 – Mazie’s Story
For the past two years Ben, Avery, our dog Riley, and I were a family of four. This all changed in September after one of those crazy days at work when one of my coworkers encouraged me to take a pregnancy test at work. The test was believed to be positive. This was a blessing to our family because we had been praying for a sister or brother for Avery. After a rough few months of emergency visits due to dehydration from morning sickness, we thought the worst was over. We welcomed the second trimester with hopeful thoughts and began to gain some weight finally after losing so much from being sick all the time. Every family that wishes to find out if it is a boy or girl looks forward to that 19-20 week ultrasound. Our family did not have a preference we just wished for a healthy baby. On the day of December 27, Ben and I awoke with excitement and met up with Ben’s parents for the ultrasound. The ultrasound seemed normal and the baby appeared to be perfect. The ultrasound technician announced she is a girl! This brought joy to my heart because Avery needs a sister. After the ultrasound appointment, we went in to the doctor’s room and waited patiently. This particular time the doctor seemed to take quite a bit longer than usual. As the doctor entered the room his face became pale and his eyes looked very worried. He then proceeded to tell us that we had something very hard to talk about. When he said those words it felt as if a wall had crashed down and felt as if a terrible nightmare had come over us. The doctor had said according to the images the baby appeared to only have a single ventricle or in other words half a heart. Our doctor being one of the best people not only medically but as a person in general began making calls to his friends that were doctors in Denver associated with Children’s Hospital and University Colorado Health. Within 24 hours we were set up with a team of cardiologist and specialist associated with Children’s Hospital Colorado. They performed an echo cardiogram and confirmed our unborn daughter did have Hypoplastic Left Heart Syndrome or otherwise known as HLHS. HLHS consists of an underdeveloped left side of the heart. As unoxygenated blood enters the right side to the heart through the Superior and Inferior Vena Cava the blood is then pumped into the lungs to become oxygenated. The blood then is brought into the left side of the heart in the Left Atria (and in a normal healthy heart is brought into the left ventricle via Mitral valve and pumped out the Aorta to be sent to the rest of the body delivering Oxygenated blood.) With our baby, her left side is underdeveloped and therefore causes the body to not receive Oxygenate blood on its own. This Congenital Heart Defect is so rare that one in 10,000 babies this happens to. We were then given three choices of either termination of the pregnancy, comfort care, or to go with a series of three surgeries. Ben and I both agreed that the series of surgeries seemed to be the best path for our baby. We were then informed that there is not much information as to life expectancy past the ages of 20-30 because until the 1980s there wasn’t any hope for babies with this syndrome. The first surgery begins roughly around day three or so after the baby is born and is known as the Norwood procedure. This requires a stent and the mixing of oxygenated blood with unoxygenated blood in the right side of the heart. The second of the series is known as the Glen procedure. This involves more stents and still encourages the mixing of oxygenated blood with unoxygenated blood. The Glen procedure is performed when the baby is approximately four to six months old. The third series of the surgeries is known as the Fontan. This involves basically bypassing the heart and delivering the blood to the body from the lungs leaving the heart as a storage facility. This procedure is performed at approximately the age of two.
We are very thankful for the amazing people around us and couldn’t be more blessed with the idea that our baby girl still has a chance. Without the help of our doctor from Banner OBGYN and the amazing team of cardiologist at Children’s Hospital of Colorado, we believe our baby girl is going to succeed on May 15, 2017.
2016 – George Thomas




My name is Candice. I am writing to your foundation, Running River Benefits, per request of a family member. First, let me tell you a little bit about our little family and secondly about our not so little situation.
My husband and I met three years ago this past May and will be married two years this coming November. My husband is an Army Veteran who did two tours in Iraq and is a Purple Heart recipient. He currently works for a local gun company in Fort Collins, American Legacy Firearms, and volunteers his time with the Military Order of the Purple Heart Chapter #434. I am currently attending the Denver School of Nursing and am on my way to receiving my bachelor’s degree in Nursing this coming December. I am currently working for University of Colorado Health-North in the float pool. I work as a CAN at Poudre Valley Hospital and at Medical Center of the Rockies.
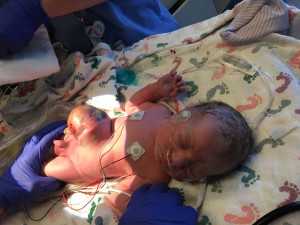
My husband and I are expecting our first child, a boy, this coming December. Interestingly enough, my due date (Dec.28th) is 10 days after my graduation date (Dec. 18th). This pregnancy has been quite a rollercoaster ride. Since I found out I was pregnant it has been a lot of visits to the doc hoping that I would stay pregnant. I was 11 weeks pregnant when I had some spotting. I called my OB and they got me in to do an ultrasound to make sure the baby was okay. That was when we found out our little man had an abnormality. After meeting with a pregnancy specialist, we found out that he has an omphalocele. The best way I can describe what an omphalocele is, is that it is a protrusion from the abdominal wall. Basically the umbilical cord did not fully close which allows intestine, stomach, and liver to sit inside a sac outside of the abdominal cavity.
We have been blessed with the specialist I have been seeing. He has been so helpful and wonderful about helping us find out how this type of abnormality can happen and what we can expect next. This type of abnormality unfortunately has many genetic/chromosomal links that can be detrimental to the fetus. Fortunately, after much testing, we have received good news. The genetic testing has come back normal and his fetal cardiac echo came back normal as well. The fetal MRI showed us that the omphalocele is mainly liver which puts the omphalocele in the large category according to the surgeon.
While my husband is covered by the VA; my step daughter and I are not therefore have private insurance. Since I am PRN I am not offered benefits, like insurance, through my work. My husband is paying for our insurance through Anthem. Being that I am healthy and so is my step daughter we went with a higher deductible for a lower monthly payment. We hoped we would get pregnant but, like many things in life we did not plan or could not plan for this.
Testing I mentioned above has been done at University Hospital and at Children’s Hospital in Denver. I see my specialist and my OB in Fort Collins. At this point we have close to $5000.00 dollars in medical bills for me and our little man. We have finally hit a point where the insurance company will pay 70/30. We have to pay $8500.00 out of pocket before insurance will pick up at 100%. However, once he is born he then has his own deductible which is also $8500.00. We have been told that with just his surgery we will hit that no problem.
I should explain more about what happens when he is born. First, he cannot be delivered vaginally and he cannot be delivered here in Loveland where we live. He must be delivered via C-section at Children’s Hospital because this is a high risk pregnancy. Once he is here, if everything goes right, the surgeon will begin the process of moving the liver back into the body and closing the omphalocele. If his lungs are not fully functioning, meaning he needs help breathing, then he cannot have the surgery right away. In fact, it could be years. This abnormality cannot fix itself and cannot be fix in utero. Again, if everything goes right, he will get to come home a month or so after he is born. However, there are multiple complications that can happen after he is born, during the surgery, and after the omphalocele is closed. One of those, which we were told was fairly common, is acid reflux. There is a possibility that he would need additional surgery to fix this. As you can imagine, his port little gut is not sitting where it should be and that can cause some issues when it comes to eating and digesting.
While this pregnancy has been difficult and challenging mentally, physically, and emotionally I would not trade it for anything. There have been multiple times where I felt that maybe God was trying to tell me that this was not going to happen but, every time I hear his heart beat and feel him move I know that he is meant to be here and that he is a fighter. He will be George Thomas the IV. My in-laws are very excited as my step daughter is their only other grandchild. My husband loves his daughter more than words can express but I know he is excited to have a little boy to watch Alabama football with every Saturday of the college football season and take hunting just like his dad too him.
We bought our house this past May and my husband is building a shed for storage in our back yard since we have all our own camping gear in the nursery right now. My step daughter said she would be willing to share her room but, I think that she would be taking that back after being woken up every couple of hours. She is so excited to have a little brother and I know she will be the best big sister George could ever hope for. My husband is an amazing man who works very hard to keep a roof over our heads and food in our mouths. Without all his love and help there is no way I would have been able to get this far in nursing school. For the first half of my program he was the only one working. Even now, I only work about 48 hours a month because of school. With drive time and class/clinical time I am gone about 40+ hours a week.
Now, we are just waiting. Waiting for him to get here, waiting for me to graduate, and waiting to see hour our bills will pan out. I won’t have maternity leave and even if I did a majority of it would be spent down at Children’s Hospital watching over our little man. My husband and I are waiting to see what happens once George is here to make a plan for him and work. It has taken a while for all this to sink in. We have had to do a lot of explaining about how we cannot bring George home right away. We are very blessed in that we have many helping hands that are willing to help with our dogs and kitties while we are in Denver with George. By far the hardest part has been all the “what ifs”; one of those being if we will get to hold him right away.
I want to thank you for considering our family in being supported by your foundation. Support in any way is needed and appreciated.
Candice & Tre
2015 – Reagan and Lillian Stewart


I have been living in Loveland with Reagan and her twin sister Lillian while my husband has been living and working in Sterling for over a year. The stress of raising twins both with health ailments has caused our marriage to be tossed aside. It has raised the question of divorce and legally separating. It has caused me to get a part time job to help offset costs and give me some much needed mommy time.
Reagan was diagnosed with atypical Hemolytic Uremic Syndrome (aHUS) at the age of 4 months. She was admitted to Children’s Hospital in Denver after not being able to pee and flu like symptoms. She went into full renal failure and had 3 rounds of dialysis, 4 pack red like cells, and 3 platelets transfusions. Her tiny little body rejected the dialysis and shred apart the transfused blood. She received her first infusion of eculizumab at 5 months of age. We are now a year into her diagnoses and she gets her infusion every Tuesday at Children’s.
She had a recent bout of fevers and viruses in January that caused another stay in the hospital. Since she now has a port for her infusions she’s at increased risk for infections.
Her infusion medicine (eculizumab, Soliris for short, the most expensive drug in the world) is $40,000 each time. We are fortunate enough to have a grant to cover some part of the cost and insurance is now starting to pick up the rest. Reagan requires on going doctor appointments with every doctor apart of her team (primary, nephrology, hematology, neurology, orthopedics, and ongoing therapy).
As far as the doctors or I can see, Reagan will receive her infusion every Tuesday for life.
There is no cure for aHUS. There is a site for aHUS and information on it. The link is http://atypicalhus.ning.com/page/what-is-ahus
I don’t have a blog set up.
Thank you for this opportunity.
Chenille Stewart
2014 – Gracie Greenlaw

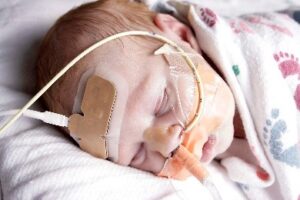
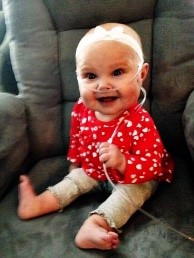
Gracie is currently 8 months old and lives with her mother, father Andy and big brother Kai (8 years old). They live in Fort Collins where Andy is a painter and Whitney is a hair stylist. Due to Gracie’s condition, she cannot be around other people or children in daycare because of the threat of her getting ill (a virus could be deadly for her). So, Whitney went from full-time work down to 2 days per week.
Here is some background history on Gracie and her condition:
On February 11, 2013 at 23 weeks pregnant the Greenlaws found out Gracie had a congenital heart defect called hypo plastic left heart syndrome (HLHS). This is the rarest and most serious heart defect. Hypo plastic left heart syndrome is a condition in which the left side of the heart, the left ventricle, either is underdeveloped or not developed at all. So sometimes it is easier to describe as having half a heart. Gracie has undergone multiple invasive surgeries, including 2 open heart surgeries- 2 few days after birth (May 30, 2013), and one on October 1, 2013. She will need at least one more open heart surgery at 2-4 years of age, and very likely could need a transplant and/or more surgeries up into her adult years to re-route her heart to function properly without the left ventricle.
Although the Greenlaw family is blessed to have insurance for Gracie, they have a $7000 deductible annually. This insurance does not cover Gracie’s monthly shots which cost over $300, prescription medication, her in-home healthcare, medical equipment that is needed in the home, 24-hour a day oxygen, weekly travel expenses to Children’s Hospital in Denver, and lost wages for hospital stays for Whitney and Andy (which could and have been weeks on end). In 2013 alone, Gracie’s medical bills and lost wages for Andy and Whitney totaled over $32,000, and their insurance premiums went up this year already. Due to a virus, Gracie was hospitalized this past December, right before Christmas, so this year is already off to a rough start. She suffered from cardiac failure and we thought we might lose her… Her heart quit functioning enough to keep her organs working on her own, so she was put on a ventilator for a few days. At that point, we had to start having talks about heart transplant. The Dr.’s didn’t think that her heart would recover from the trauma. Since December she has been slowly improving, she is still technically in heart failure, but we are hoping that she will continue to improve. . With just one little bug, she can get so sick. The same illness that would have a normal child in bed with fever for 3 days could kill Gracie. We are currently paying our $7000 deductible for this year. We are making about $650/ month for the next few months and about $600/ month in other medical expenses. (Medicines, oxygen supplies, pules ox rentals, and home nursing charges) as well as gas to and from the hospital. We are only having to go down about once a month now which is great! After the deductible is payed off, we will still have the $600/ month of uncovered medical expenses.
With all of this explanation, my point is to humbly request that your foundation sponsor Gracie and her family. It is SO VERY important that she stays healthy, and I am a firm believer that a happy, stress-free (as much as possible in this situation) home can do wonders for a child and aid in her healing and thriving. Bills and money issues cause stress, and it’s just one more thing these awesome people should not have to worry about just because their precious baby is sick. I admire them so much and would be grateful for any help you might be able to offer them.
God bless you and yours.
2013 – Nicholas Smotherman


Nicholas Smotherman was born March 22nd 2011. When Nicholas was born they right away noticed that he was a very “calm” baby. We had to give him sugar water right away to help him get some movement going. The urologist noticed that he had a blockage in his urethra. We would have to do surgery at a month old. 2 days later Nicholas developed a 104* degree fever. At the hospital they did multiple test, CT scans, spinal tests, blood work, x-rays, all kinds of things. They diagnosed him with a UTI, RSV, Spinal meningitis, severe acid reflux, severe low tone and they noticed that he had a lot of fluid around his brain. We soon met with the neurologist who wanted to do many more tests on Nicholas because of his low tone and activity level. We did test on anything and everything but the one thing that she thought for sure would be positive would be a syndrome called Prader Willi. A syndrome where the body can’t consume enough food. Conducted CT and MRI scans of his brain. (He was around 5-6 months at this time now) Nicholas has a very large head and that worried those because of the fluid around his brain. Nicholas also started having what looked to be like seizures so we had to do some EEG studies. When they did the CT and MRI scans they noticed that his brain isn’t growing like it should. From April to Sept there had been NO growth at all and that worried them. We met with a metabolic specialist who once again said we believe your son has Prader Willi and may need a shunt in his head to help relieve pressure from the fluid and let the brain grow properly. About 2 months down the road the tests for Prader Willi came back and they were NEGATIVE. We went and saw a Prader Willi specialist we were discussing his bones and his movements and his feeding problems. Despite the fact of all Nicholas’ blood work for Prader Willi there are cases where the blood is actually false positive. Four doctors still believe Nicholas has Prader Willi which then will be a lifetime of therapy, and diets and discipline.
They have decided to wait until June of 2013 to do his final MRI and see if he has any change in his brain.
With his problems with his GI system they noticed that he was always gagging and spitting up. We went ahead and did what’s called a PH probe and that measures the acid in Nicholas’ esophagus, low and behold it was severe. So severe it was actually eating away his esophagus. They put Nicholas on an adult strength medicine. He has been on the acid medicine every day twice a day for about a year. The GI doctor decided that the best thing to do would be to do a G-tube and a surgery called a Nissan Fundoplication. That is where they go in and cut the stomach muscles and tie them tighter around the sphincter and make it so things don’t come up. We go see the doctor April 15th to talk about scheduling this surgery. They will also be putting a G-tube in him to help relieve gas and since Nicholas isn’t gaining weight properly to help him eat.
Nicholas was diagnosed with asthma as well. Last year he got croup 6 times, he has had RSV 3 times and pneumonia 5 times!! He is on a daily dose of an inhaler. Nicholas has had over 100 blood draws in his life, many procedures and many more to come. We do therapy 3 times a week for an hour to work on muscle tone and eating and speech! He is on 11 meds a day, and we are adding a few more to help get the muscles on track. Thank you for listening to my story. Lindsey Smotherman the mother of a beautiful son!!!
Right now we pay $1700.00 a month for health insurance and sometimes we have to not pay a house payment to make sure we pay that! I can’t let Nicholas be without insurance. We owe over $9000.00 to collection agencies because of all the hospital stays and medicines and doctor apts. We spend about $500.00 a month on medicine for Nicholas. We have many more surgeries and test and hospital stays coming up in the near future.
2012 – Corbin Gaines
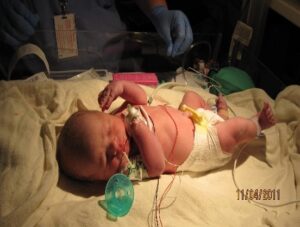
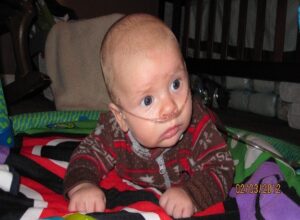
Corbin Gaines was born on November 4th, 2011. He was born premature at 36 weeks 5 days. At 4 weeks of age he was diagnosed with tracheomalacia- softening of the airways. He was placed on acid reflux medication to prevent any further damage of the trachea and esophagus. At about 6 weeks of age we noticed he was having a very hard time breathing and was turning pale. He was aspirating milk and liquid medications, and was frequently choking and vomiting because of his suspected tracheomalacia. His pediatrician ordered a home sleep ox study and they monitored his oxygen levels for 24 hours. She placed him on 24/7 oxygen because his oxygen levels were consistently low. She also recommended that he receive a monthly shot of synagis, which would protect him from RSV. The insurance has not approved it thus far as the shots cost approximately 3,000 dollars each. We are in the process of working with them to appeal the decision.
He recently had a visit with a pulmonologist at Children’s Hospital in Aurora, CO. She ordered a sleep study, barium swallow, an upper gastrointestinal series, and a bronchoscopy, all to be done within the next month. Each procedure requires at least a 23 hour observational stay at the hospital for monitoring. He also has to have a certain diet- mom has to eat no dairy, chocolate, caffeine or any high fiber products to reduce the amount of gas he gets. Due to his condition he swallows too much air and this puts pressure on his diaphragm causing him to have an even harder time breathing. He had his sleep study on Friday the 10th of February where we stayed overnight at Children’s Hospital. He was diagnosed with severe sleep apnea (absence of breathing), and severe laryngomalacia (softening of the larynx). They had him on room air and noticed that his oxygen levels were severely low for long periods of time. The sleep doctor as well as his pulmonologist recommended that he see an Ear/Nose/Throat specialist which he will see on the 29th of February at Children’s Hospital. They are all recommending that he be a candidate for a new surgery that would strengthen the trachea/larynx. This surgery might possibly include the pulmonologist, ENT specialist, and cardiologist to all be present. They believe he might have a loose airway, or even a possible obstruction that will require a laryngoplasty.
For now he is on constant oxygen and is preparing for at least one or more appointments per week at Children’s Hospital for the next two months. His supplemental oxygen helps him maintain good levels of oxygen at night, but he still wakes up 4-5 times a night because he has trouble breathing. His acid reflux is getting better now that his medication is regulated. Despite his medical issues, he’s a happy growing baby with a great attitude about all his appointments.
Chase, Chelsea, and Corbin Gaines
2012 – Zoie Cissell


Zoie was born in May of 2011, and is almost 8 months old now. She was born via C-section due to some poor growth the last few weeks, and arrived 3 weeks early. She came out healthy, but only weighed 5 pounds and was 17 inches long.
When Zoie was 6 Weeks old, her parents received the news from a newborn screen test that she had Cystic Fibrosis, a lung disease. They would learn through monthly checkups at Children’s Hospital how to keep Zoie as healthy as possible, keep her away from pets and smoke, and all the extra vitamins she would need.
At 10 Weeks old, on a family trip to Nebraska, Zoie had her first seizure. Sent by ambulance on a 5 hour drive to Children’s in Denver, the family spent 5 days while Zoie was diagnosed with microcephaly, or small head syndrome, and epilepsy. She also had caught meningitis. This was the family’s first long stay at Children’s, while Zoie underwent an MRI, spinal, and met her geneticist, and neurology team for the first time.
Zoie managed to be seizure free for two months, but then her episodes started getting worse and were happening every day. She got hospitalized for two Weeks while the doctors tried to get control of her seizures. They sent the family home with Zoie having one every 3 days. I am now proud to say that we are down to about one every two Weeks.
Zoie recently also caught a strain of RSV and was put in the hospital for 4 days until her lungs cleared up. She was only 10.12 pounds, and dropped down to 9.13 pounds. She is very healthy now, but we are working on some weight gain for her so that we don’t have to do a G Tube, or feeding tube. If you see Zoie, you would never know what she has been through or will continue to go through. She is the happiest baby out there and continues to do well in her PT and OT. Her dad works hard so her mom can stay at home and make sure she gets the best care possible. We never know what tomorrow may hold, but we wouldn’t change our life for anything. Zoie has taught hundreds of people how to live life and live it with a smile and God by your side. If you want to learn more about Zoie, visit her caring bridge site at Caringbridge.com. Her site name is Zoieraecissell.
Thanks for listening to our story
Love from the Cissell’s
2011 – Macy Helm

In June 2009 when Macy was 3.5, Brandon and I noticed that her eyes were swollen. We went to the pediatrician who treated her for allergies.
A couple of weeks later while on vacation in Kansas City she started to swell in her stomach and legs. We went to Children’s Mercy Hospital where she was diagnosed with Minimal Change Nephrotic Syndrome.
It is an autoimmune disease in which the white blood cells produce a substance that causes the kidneys to spill protein into her pee. When she doesn’t have enough protein in her blood, the tissue takes on fluid and she swells. It also, over time, causes scarring on her kidneys.
Several immunosuppressive medications like Prednisone and chemotherapy drugs help some people’s kidney’s stop spilling protein and put them into remission. Unfortunately, no medications have worked for Macy since January 2010. Last December a kidney biopsy confirmed that she has FSGS (Focal Segmental Glomerulosclorosis) a degenerative form of Nephrotic Syndrome.
Macy has spent nearly 50% of the past two years in the hospital for edema, blood clots, infections and kidney failure.
She is now 5 and has end stage renal disease. In April, she was placed on peritoneal dialysis which she does at home each night. In May, she had both of her native kidneys surgically removed, in order to stop protein from spilling into her urine. This June, we will travel to Chicago where Macy will have a kidney transplant. A transplant, unfortunately, is not a cure for FSGS and it could recur in her new kidney. Since she is so young, she will eventually need another kidney transplant.
For now, we pray a new kidney will give her a “normal” childhood. If you would like to follow Macy’s story visit our caring bridge site www.caringbridge.org/visit/macyhelm
I had also just made a video about Macy’s story to help raise money for a walk we do each year for the NephCure Foundation you are more than welcome to watch/share.
2010 – Tragedy for the Thompson Family
Dustin and Janice were starting a family, they were celebrating the birthday of their 1 yr. old son this Saturday. They were also trying for their second child. Janice thought she may be pregnant and was waiting for Dustin to get home from a family vacation so they could take the test together.
Tragically Dustin was killed in a roll-over accident on I-70. As it turns out, Janice is in fact pregnant with their second child. They are friends of mine, but even if they weren’t they share a common bond with me and those of us with young families. I was devastated when I heard the news, but it could not compare to the life changing impact it would have on Dustin’s family and mostly Janice.
2010 – Trenten Viney
Twenty-one-month-old Trenton Viney suffered massive burns Wednesday after the family dog apparently knocked a can of gasoline into a space heater in a garage, family members said.
His father, Josh Viney, was burned as he grabbed Trent and raced outside of the blazing garage. Josh Viney was cleaning the engine of a vehicle inside their garage while Trent played nearby, said cousin Heidi Collins.
Josh Viney and his partner, Alex, Trent’s mother, flew with their son Wednesday night to California and are holding vigil at the Shriners Hospitals for Children-Northern California in Sacramento, Collins said.
“They don’t really know what the prognosis is,” she said. “They just want their baby to be OK.”
Neighbors reported hearing a popping sound just before noon Wednesday, saw smoke pouring from the duplex’s west-side garage and then saw Josh Viney run outside cradling Trent.
Collins said Josh Viney suffered serious burns but is only thinking of his son.
“He’s distraught. He doesn’t know what to do,” she said.
Fire investigators have ruled the cause accidental. The duplex has been boarded up; the fire destroyed the garage and damaged the living areas of the home on the 900 block of Camelot Court.
Collins said Josh and Alex don’t have a lot of money and are now staying in a strange city far from home without many resources. She said Trenton’s extended family is trying to raise donations to help pay for a hotel room near the hospital.
“We just want to help them not worry about anything else in Sacramento,” she said.
A cash-assistance fund has been set up in the name of Trenton Viney. Donations are being accepted at any Home State Bank.
This story written by Trevor Hughes, Fort Collins Coloradoan.
2009 – Children’s Hospital